By Melissa Walsh
When Bianca Savage noticed some worrying symptoms with her youngest son Mason she naturally became concerned. It was a gradual process at first, with her active 10 year old suddenly displaying extreme exhaustion when playing football, drinking more water and going to the toilet on a more regular basis.
“I had no idea what was wrong with him but I knew there was something. He was tired and irritable and very pale. I remember one day at football, he drank all my bottle of water and his and was still thirsty. He was also going to the bathroom a lot,” said Bianca. “He would have to rest for long periods after he’d played only a small amount of football and he seemed to have lost his appetite.”
It was 13 July last year that Bianca and the family were given the diagnosis that Mason had Type 1 Diabetes, and it shook them to their core.
“In the three weeks leading up to that his symptoms got so much worse. He was drinking all the time, losing weight and going to the toilet more than anyone should need to and even wetting the bed which he had never done before. I knew there was something seriously wrong but the first doctor we took him to said it was probably an inner ear problem,” said Bianca, who then found Mason displaying other symptoms. “One day he called me into his room and said his eyes felt weird. He had his eyes closed but they were still moving.”
Within eight days of the original doctor’s appointment, Bianca had Mason went back at her regular family doctor who diagnosed Mason on the spot.
“I remember how shocked I was when he said he suspected Mason had Type 1 diabetes. I thought ‘there’s no way; he is too young’. Then I realised I knew nothing about it and was confused with the Type 2 kind,” she said. “He took a blood sample and his level was extremely high so we packed a bag and went to the hospital where he spent the next week learning about Type 1 diabetes and trying to manage his levels.”
For mum of three, Bianca, the diagnosis was a complete shock and something the family is still learning to cope with.
“We really didn’t know anything about it and of course I was really worried because of the state of my son’s health and the fact he would be insulin dependent,” said Bianca, who then learnt that Type 1 diabetes is when the pancreas no longer produces insulin, a hormone your cells use to turn sugar into energy.
She discovered quickly that Mason must take insulin, either by injection or through a pump attached to the body, to keep blood sugar levels in range in efforts to avoid serious long-term complications such as kidney failure, heart disease, lower-limb amputations, and blindness. “Mason has a lot of anxieties and he didn’t cope with all this information. It took three of us to hold him down to give him the insulin, and it was absolutely horrible.”
Bianca says that, even a year later, they’re still learning about the diagnosis and living with it every day.
“At the hospital there is the diabetes clinic and the educators are great. They step back when they can see your brain is getting overloaded with information. They gave us lots of information to read but one of the best books I go to is one they gave to Mason called ‘Frances learns about Diabetes’. It is simple and explains everything in clear terms. Every time I get overwhelmed I go to it and read it. I take a breath and realise this is something I can do.”
It has been a long road for the Savage family since July last year with everyone having to adjust but Bianca says the toughest part is remaining positive.
“Mason has missed a lot of school since last year, and just had another stint in hospital to get his levels stabilised,” she said. “However these days he does the injecting himself and is getting very good at it.”
For Mason to keep on top of his levels, he has to do a blood test four times a day and self-inject at breakfast, lunch, dinner and before bed.
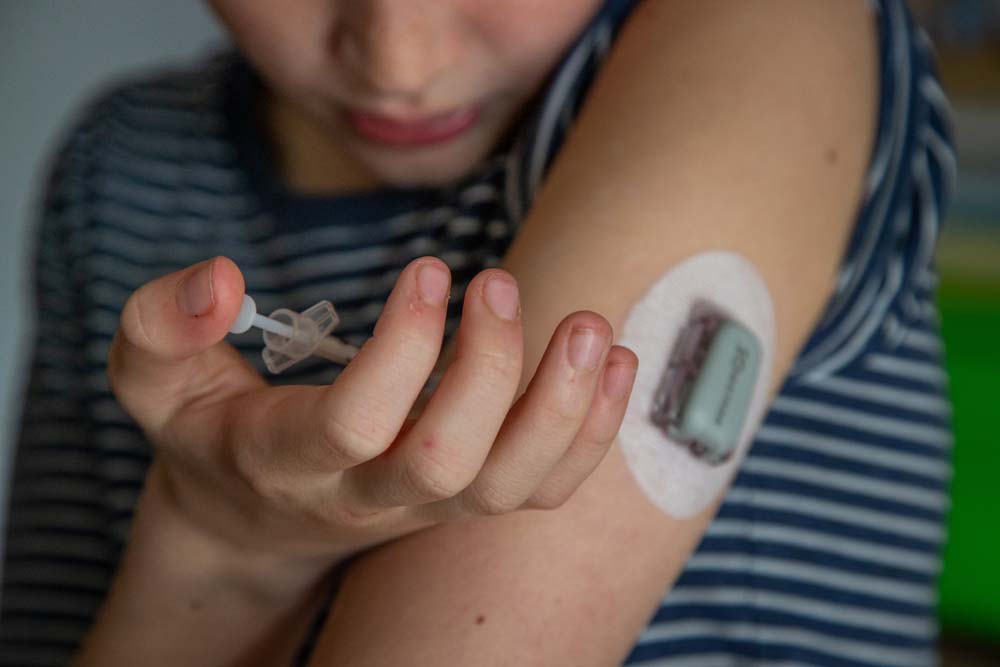
“It doesn’t really hurt when I do it and I use different arms and my legs each time to make sure I don’t get scar build up,” said Mason, who shows us how to do the “inject and blood” test while we are there.
For the grade four student, part of the management is to eat small, frequent meals.

“I eat six meals a day that mum or my family make for me,” said Mason.
“With his food, it has to be one to three serves of carbohydrates in each meal and about two hours apart,” said Bianca, who visits the dietitian clinic every Thursday for advice and guidance.
“I think the food is one of the hardest things as it makes all the difference in his insulin levels,” said Bianca.
One thing that has made the process easier is a machine they started using five months ago called a Dexcom.
“It is a blood sugar measure that sends the readings via Bluetooth to my phone and his. It means I can check his levels at any time during the day, particularly if he is at school,” said Bianca.
The Dexcom is a small device that is attached to Mason’s arm and has a chip that records the blood sugar readings.
“I can click on it anytime during the day to check his reading, and the main aim is to get the insulin to stabilise enough so that he is in the grey zone,” said Bianca. “That means he must have a reading between four and 10; anything above is hyper and anything below is hypo.”
While a Type 1 diabetes diagnosis can be hard to process, Bianca says one of the best pieces of advice came from an educator at the diabetes clinic.
“Diabetes changes your family life. At first it was really hard and I was trying to be so regimented with it, trying to make our life fit around diabetes. One day when I spoke to the diabetes educator, they said, ‘Relax. What needs to happen is diabetes needs to work around our life, and you are not to live every moment about the illness.’ When we were first diagnosed we stopped doing social things like going out for dinner. Mason hated injecting in front of people and he had to eat at certain times. I was very hard on myself if I missed something in his care so that was a big hurdle to get over. I would write everything down and was so hard on myself because if he doesn’t get the insulin he dies and that’s a fact. These days, we are a little easier on ourselves and realise that occasionally we can lighten up a bit.”
With a family dynamic involving two other siblings, life can go back to some normality for the Savages.
“It helps having two older siblings for Mason as they have other stuff going on. I also work five jobs with our timber window manufacturing business. I work at a gym crèche, a kindergarten, do some nannying and a cleaning job,” said Bianca, who like any mum is trying to keep everything running smoothly. “Understanding diabetes is part of the key as well as educating people. We know this is for life and they are working on advancements all the time but at the moment it is a day by day process that we are learning about all the time.”
Diabetes is one of the most misunderstood health conditions. To clear the public confusion about what is and isn’t true, Diabetes Victoria launched a new ‘Bust a Myth’ campaign in early June, debunking the top five myths around living with diabetes.